Introduction
Peripheral nerve tumors can occur anywhere in the body. Most of them aren't cancerous ...
When mesh leads to complications
Operations involving the implantation of plastic bands or nets, the so-called "mesh", in the pelvis involve the risk of nerve injury - especially of the pudendal nerve and the so-called sacral roots. Pelvic nerve damage can also occur during surgery due to coagulation, suturing, lack of blood supply (ischemia) or cuts. They cause feelings of irritation or numbness, burning pain and dysfunction, which occur immediately after the operation or after a few days. Such injuries of the pelvic nerves occur much more frequently than is currently assumed.
Complications do not necessarily only appear immediately following mesh implantation. The direct implantation of mesh material on pelvic nerves but also sutures, bruises or abscesses may lead to nerve complications which manifest themselves in severe nerve pain immediately after the operation. A nerve compression caused by scar tissue (fibrotic entrapment) or a nerve compression caused by constriction due to enlarged blood vessels in the pelvis (vascular entrapment) can develop over several months or even years. The characteristic pain does not occur immediately following surgery, but months or years later.
The transvaginal fixation of the vaginal stump (lowering operation) is a classic procedure that involves a high risk of injury to the pudendal nerve. The damage can be caused by a direct lesion of the nerve (a bruise) on the posterior part of the pelvis between the sacrum and the ischium, or by a pinching of the nerve if a haematoma or abscess develops. Newer treatment methods that use mesh material to fix the pelvic organs (vagina, uterus, intestine) to the sacrum can also increase the risk of nerve damage for the patient.
The most common symptoms after damage to the pelvic nerves are:
Neuropathic pain (nerve pain) resulting from injury to the pelvic nerves is described as an excruciating "burning pain" or "electrical pain". This type of pain manifests itself in the back part of the thigh (dorsal) and may reach as far as the foot, the region around the anus and sphincter muscle (perianal region), the genital region, the buttocks, the lower back or the inside or outside of the thighs.
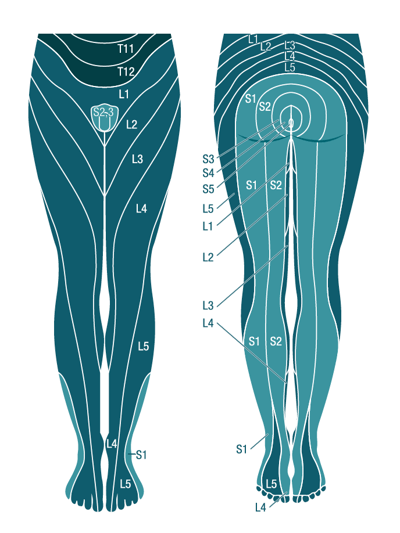
The pudendal nerve is of particular importance for the function of the pelvic floor muscles, sphincters and genitals. If it is injured directly, it causes pudendal pain, i.e. severe pain in the genital and perineal area, usually unilateral, and possibly erectile dysfunction in men as well as urinary incontinence if the lesion is bilateral. Surgical nerve damage can therefore not only trigger pudendal neuralgia, but also lead to urinary or faecal incontinence and sexual dysfunction (erectile dysfunction).
If, on the other hand, the pudendal nerve is irritated only by a pathological proliferation of the connective tissue (fibrotic entrapment) or if there is an entrapment by pelvic blood vessels (vascular entrapment), this leads to the same pain and also occasionally to sexual disorders, hyperactivity or hypersensitivity of the bladder and/or intestines.
Difficult diagnosis due to delayed onset of symptoms
Since the pain and dysfunctions caused by nerve injuries develop during surgery immediately after the operation, a possible surgical complication can be detected at an early stage by both the surgeon and the patient. The result is a new operation with the aim of repairing the damage immediately.
If, however, the mesh implantation has caused a proliferation of the connective tissue and thus an entrapment of the pelvic nerves (fibrotic entrapment), the situation is much more difficult. Since the pain can only appear after several months or years, the link with the procedure is not immediately apparent. The diagnosis is further complicated by the fact that the neuropathic pain is not located in the pelvis, but further away in the back, buttocks, pudendal region or lower extremities. All these pain points are usually associated with orthopaedic or neurosurgical causes.
Relief of symptoms by releasing the nerves
If an injury to the pelvic nerves is diagnosed, a thorough clinical evaluation and a more precise diagnosis are indispensable. First, the injured nerve must be accurately identified. In the next treatment step, laparoscopic exploration can be considered. The area is inspected meticulously with the help of a tiny camera. This enables an exact diagnosis of the cause. In the same treatment step, decompression of the affected nerves must be achieved by releasing the nerves. The aim of the intervention is not the removal of the mesh (reduction of recurrence!), but the complete liberation of the nerve. As the pelvic nerves, as the name suggests, are located inside the pelvis, such an operation cannot be performed through the vagina, as this would only allow the removal of the mesh but not the liberation of the nerve. Systematic exploration of the damaged nerves by laparoscopy is required.
Another therapeutic option - if the nerves are severely injured or destroyed - is the implantation of electrodes for neuromodulation in the case of nerve injuries, but this is used in less than 5% of patients.
If necessary, the mesh can be removed laparoscopically through small openings in the abdominal wall and a tiny camera. The laparoscopic examination must be performed as soon as possible before irreversible nerve damage occurs and the pain becomes chronic.
Precision diagnostics are carried out at the Possover International Medical Center. Mesh removal is performed using innovative minimally invasive techniques. Prof. Possover is one of the few surgeons worldwide who can remove mesh laparoscopically. The treatment results in a clear relief of the discomfort for the affected women.
To help people in difficult situations to improve their quality of life has become his life's passion. Continuous research, decades of clinical experience and the focused determination to find a solution for previously unsolved medical problems, have enabled Prof. Possover to help often quite discouraged patients find release from their seemingly insurmountable problems.
Our team will take care of you
We will dedicate our expertise and know-how to help you find the solution that is right for you.
„As a cheerful, open and communicative person, I really appreciate coming into contact with people from all over the world. The well-being of others is very important to me.“
If it is your preference, your attending doctor is welcome to accompany you to Zürich. You will then have a person at your side who is familiar with your medical concerns. At the same time, your doctor will have the opportunity to be present during the planned operation and gain unique insights into the applied practice of Neuropelveology.
Neuropelveology is a medical discipline developed by Prof. Possover. It is based on the discovery of the pelvic nerves and includes the diagnosis of the diseases of these nerves by means of gynaecological examination methods and their treatment by means of laparoscopy.
Read morePeripheral nerve tumors can occur anywhere in the body. Most of them aren't cancerous ...
Vulvodynia is a chronic pain syndrome affecting respectively the vulva and occurs ...
The discipline of Neuropelveology, founded by Prof. Possover, offers new diagnostic and therapeutic possibilities in ...
If women suffer from cyclical sciatica with onset of numbness in the buttocks or legs, or experience movement ...
Klausstrasse 4
CH - 8008 Zürich
Switzerland
E-Mail: mail@possover.com
Tel.: +41 44 520 36 00